NEWSLETTER
Eyes FORWARD
Cataracts – Part 1: Choosing When To Proceed With Surgery
Volume 01
While cataracts might not sound like an exhilarating topic, hang in there with me because we are going to spice this up and make it fun. Rather than breaking down the types of cataracts and the underlying factors that lead to cataract formation, I would much rather talk to you about how a medical practice iagnoses cataracts, how we decide when to treat them and how we arrive at the decision of choosing the proper intraocular lens (IOL) for the patient.
Throughout my career, when lecturing on this subject or speaking with referring doctors, the recurring thought process conveyed back to me was mostly centered around when cataracts are “ripe” (I always loved that term). Well, when something is ripe, you pick it. Right? Maybe. Let’s explore this a little further. First of all, what metric drives (or justifies) a referral for a cataract evaluation?
- Does best-corrected distance visual acuity (BCDVA) in the affected eye(s) have to drop to 20/50 or worse?
- Does the physical appearance of the opacity (nuclear sclerosis, cortical spoking, posterior subcapsular, other) have to progress to a specific grade?
- Does the patient have to provide an unsolicited complaint about how the cataract is affecting their vision, whether that be a reduction in acuity, increased difficulty night driving, etc.?
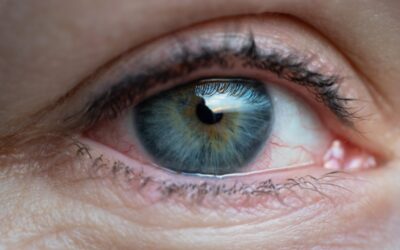
While we look at these things too, I want to invite you to look at all of this and then add the following additional thoughts to your overall calculus. Consider this… the glare caused by the presence of cataracts can be disabling in bright light conditions due to light scattering as it passes through the cloudy lens. The Brightness Acuity Test, generally referred to as the “BAT” test, is designed to test and quantify just how debilitating glare is to the patient. The BAT test has three settings that are designed to simulate the effect of common lighting conditions (direct overhead sunlight, partly cloudy day, and bright overhead commercial lighting). If the patient’s vision gets worse while using the BAT, then we need to consider that the patient has a glare disability. Pretty simple when you phrase it like that.
Now, what does this mean clinically? What we very often see here in clinic is a patient whose BCDVA is, let’s say, 20/30 (which would not seem to qualify for cataract surgery), but when you BAT test them, they drop to 20/60 (which does qualify). When you ask these people questions like, “Do you have trouble driving at night?”, they will often say things back to you like “Oh, I don’t drive at night anymore”, or “Yeah, it bothers me a lot, so I try to avoid it”. This should be a revelation to us all. Here we have a patient that, I dare say, many providers would look at and think that they are not ready for surgery. I would argue that if they BAT to 20/50 or worse and they have a complaint to justify treatment, then I would recommend that they start thinking about, and preparing for, cataract surgery. I would also add that the younger a patient is, the softer the cataract, the easier it is to remove it, and the faster they will heal from it. All important factors to add to your calculus.
Okay, so now the decision to do cataract surgery has been made. Now what? Well, I believe very strongly that the next step is of crucial importance. This decision will affect them for the rest of their life. Let that sink in. Think about the gravity of this decision. What intraocular lens (IOL) should be chosen? Monofocal? Toric? Multifocal? Extended depth of focus? What should be the aim? Distance
OU? Monovision? That is a very deep and important well and I think these questions are deserving of their own newsletter, so stay tuned for part 2 of the cataract journey. Coming soon!
Until next time!
George Goodman, OD, FAAO
Director of Cataract and Refractive Services
EyeCare Associates of South Tulsa
10010 E 81st St #100, Tulsa, OK 74133
O: 918.250.2020 | C: 405-245-9333 | F: 918.250.8910
www.southtulsaeye.com
Service-oriented, comprehensive eye care in a timely fashion.
Please send your comments and suggestions to DrGoodman@southtulsaeye.com
or call Dr. Goodman at (405) 245-9333 (cell).
Missed a newsletter? Find them below.
Can Dry Eye Cause Blurry Vision?
Dry eyes are often caused by an imbalance in the tear film on the surface of the eye. This causes irritation that leads to inflammation and damage to the cornea. The most common symptom is blurred vision. Other symptoms include burning, itching, redness, and...
Implantable Collamer Lenses (ICLs) – 08
NEWSLETTER Eyes FORWARD Implantable Collamer Lenses (ICL) Volume 08 We hope that you’re enjoying our newsletters. In this edition we are going to discuss Implantable Collamer Lenses (ICLs). An ICL is a posterior chamber phakic intraocular lens (pIOL). To be more...
Refractive Lens Exchange (RLE) – 07
NEWSLETTER Eyes FORWARD Refractive Lens Exchange (RLE) Volume 07 “A rose by any other name would smell as sweet.” Thank you Mr. Shakespeare! Speaking of names, “Refractive Lens Exchange” is known by numerous monikers. Let’s see… (1) Clear Lensectomy, (2) Refractive...
Contact Lens De-adaptation – 06
NEWSLETTER Eyes FORWARD Contact Lens De-adaptation Volume 06 Thank you for the support and welcome back! In this newsletter, we are focusing our attention on contact lens de-adaptation. While this may not sound very interesting, I promise you it is… and it is vitally...
Eyes Forward – Laser Floater Treatment – Technology Matters – 05
NEWSLETTER Eyes FORWARD Laser Floater Treatment – Technology Matters Volume 05 Welcome back! We are all very excited about this second edition of Eyes Forward where we get to talk about Laser Floater Treatment (LFT). LFT, also known as Laser Vitreolysis, is a...
Eyes Forward – Laser Vision Correction – Technology Matters – 04
NEWSLETTER Eyes FORWARD Laser Vision Correction: Technology Matters! Volume 04 In this First Edition of our newly minted newsletter, we will focus on Laser Vision Correction (LVC) and discuss the best technology available… and more importantly… why it is the best. As...