NEWSLETTER
Eyes FORWARD
Contact Lens De-adaptation
Volume 06
Thank you for the support and welcome back! In this newsletter, we are focusing our attention on contact lens de-adaptation. While this may not sound very interesting, I promise you it is… and it is vitally important to achieving optimal outcomes in all forms of refractive surgery. This topic has been a source of much debate in refractive surgery circles for decades because it affects surgical outcomes, so we need to factually sort this out and get this one right. The reason I want to cover this topic is to make sure that the salient points of this debate are laid bare so we can begin to look at this as we should be looking at this. What does that mean? Stick with me and you will soon know all you need to know.
Let’s start with a basic question: What are we trying to accomplish through contact lens de-adaptation? Are we overtly trying to inconvenience a patient and delay their surgery? Absolutely not! I would argue strongly that we are striving to achieve homeostasis so we can ultimately give them the best outcome possible. Getting a person back to their natural “unadulterated” state so that they can be properly measured, is the best approach in the goal of obtaining stable biometry. The term “garbage in… garbage out” is so applicable here. Rushing a contact lens wearer to surgery is wrong because their eye is not yet stable in key areas such as hydration, topography, oxygenation, aberration, pachymetry, etc. I would dare say that rushing a patient to surgery before stabilization is outright unethical! Centers that rush this and don’t allow for proper stabilization are broadcasting that they just don’t care about anything but their bottom line… or they just don’t understand the importance of this topic (or likely both). Either way, you should understand these things so you can feel better about where you refer… and why! I’ve often said to patients that I don’t want to intentionally inconvenience them, but if it means giving them a better outcome, then that is what I am focused on. Medical appropriateness always outweighs convenience! Rarely is this stance not received well by a prospective patient. They NEED to know that we care most about their safety and the quality of their outcome.
Another question: What is more important… the timeline for being out of contacts, or achieving overall biometric stability? I hope that this one is obvious. Stability is everything! Good biometry leads to the best results. If an eye is dry before surgery, then treat it and bring about normalcy, and then proceed. If topography is distorted because of contact lens abuse/over wear, then stay out of the contact lenses until the topography stabilizes/normalizes, the refraction is repeatable and the ocular surface is controlled and quiet, and then proceed. In this clinic, we boast of having a less than 1% enhancement rate with laser vision correction (compared to 4% nationally), and that statistic being so low is not by accident. It is by watching and insisting on the pursuit of perfection. In the long run, this approach saves time and money, minimizes risks, and builds a great practice with lots of great reviews and a high referral rate. When you heart is in the right place and your priorities are in line… excellence follows.
So, now that we’ve made our case as to why sufficient de-adaptation is crucial, what is it that we are specifically recommending from a timeline standpoint? Here are my thoughts on that:
Soft Contacts Lenses (SCLs)
- If topography is pretty normal/regular at the initial consultation visit, then we insist on at least a week out of SCLs before any pre-operative measurements are taken.
- If topography is irregular, abnormal, suspect, etc., then we will wait at least 2 weeks before bringing them back for evaluation, repeat topography and treat them for any underlying condition that may be contributing to their instability. Once stable, we determine candidacy and proceed as reasonable.
- If dryness is present, then we will aggressively treat the ocular surface (PFATs, gels, ointments, etc.) to improve overall health. We will also consider adding oral omega-3 (2000mg/day) if oil expression is not optimal.
- If allergies are present, then we prescribe a topical antihistamine and consider adding an oral, depending on severity.
- If there is a history of eye rubbing, then we discuss the long-term risks of eye rubbing leading to corneal destabilization, ectasia and possible PKP and urge them to change this behavior for their long term eye health.
Rigid Gas Permeable Lenses (RGPs)
- Proper RGP de-adaptation greatly reduces risk for enhancement!
- Minimum time out of lenses is 6 weeks, or up to 1 month per decade of wear, whichever is greater. We repeat topography every 2-4 weeks until stable.
- The most important factors to consider are topographic and refractive stability. Once achieved, we can assess candidacy and proceed as reasonable.
- After long-term RGP wear, some corneas never return to their natural, pre-RGP state, so we must be certain that these corneas settle into their final shape and then assess them for any abnormalities before proceeding.
- If SCLs are chosen as the vehicle for RGP de-adaptation, then the RGP de-adaptation guidelines must be met first, followed by the proper SCL de-adaption guidelines thereafter.
Please know that this same logic applies to any and all refractive procedures. While LASIK and PRK patients benefit from these de-adaptation guidelines, so do Implantable Contact Lens patients (ICLs), Refractive Lensectomy patients (RLEs) and cataract patients (especially when dealing with premium IOLs)!
Key thoughts:
- A guiding principle in my life: “It takes longer to explain why you didn’t do it right the first time”
- Great biometry leads to great results! We take the time, and we do the job right… the first time! You can refer with confidence!
Until next time!
George Goodman, OD, FAAO
Director of Cataract and Refractive Services
EyeCare Associates of South Tulsa
10010 E 81st St #100, Tulsa, OK 74133
O: 918.250.2020 | C: 405-245-9333 | F: 918.250.8910
www.southtulsaeye.com
Service-oriented, comprehensive eye care in a timely fashion.
Please send your comments and suggestions to DrGoodman@southtulsaeye.com
or call Dr. Goodman at (405) 245-9333 (cell).
Missed a newsletter? Find them below.
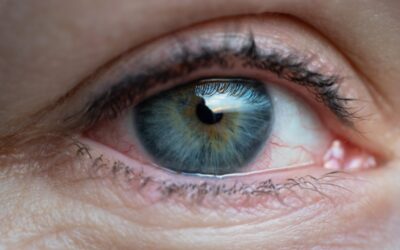
Can Dry Eye Cause Blurry Vision?
Dry eyes are often caused by an imbalance in the tear film on the surface of the eye. This causes irritation that leads to inflammation and damage to the cornea. The most common symptom is blurred vision. Other symptoms include burning, itching, redness, and...
Implantable Collamer Lenses (ICLs) – 08
NEWSLETTER Eyes FORWARD Implantable Collamer Lenses (ICL) Volume 08 We hope that you’re enjoying our newsletters. In this edition we are going to discuss Implantable Collamer Lenses (ICLs). An ICL is a posterior chamber phakic intraocular lens (pIOL). To be more...
Refractive Lens Exchange (RLE) – 07
NEWSLETTER Eyes FORWARD Refractive Lens Exchange (RLE) Volume 07 “A rose by any other name would smell as sweet.” Thank you Mr. Shakespeare! Speaking of names, “Refractive Lens Exchange” is known by numerous monikers. Let’s see… (1) Clear Lensectomy, (2) Refractive...
Eyes Forward – Laser Floater Treatment – Technology Matters – 05
NEWSLETTER Eyes FORWARD Laser Floater Treatment – Technology Matters Volume 05 Welcome back! We are all very excited about this second edition of Eyes Forward where we get to talk about Laser Floater Treatment (LFT). LFT, also known as Laser Vitreolysis, is a...
Eyes Forward – Laser Vision Correction – Technology Matters – 04
NEWSLETTER Eyes FORWARD Laser Vision Correction: Technology Matters! Volume 04 In this First Edition of our newly minted newsletter, we will focus on Laser Vision Correction (LVC) and discuss the best technology available… and more importantly… why it is the best. As...
Cataracts – Part 3: Dropless Cataract Surgery – 03
NEWSLETTER Eyes FORWARD Cataracts – Part 1: Choosing When To Proceed With Surgery Volume 03 “To drop, or not to drop: that is the question.” In recent years, “Dropless” cataract surgery (intracameral injection) has gained in popularity… and for very good reason. When...